June 19 is World Sickle Cell Day, an international awareness day aimed at increasing the public’s knowledge and understanding of sickle cell disease and its challenges. Sickle cell anemia is a painful hereditary blood disorder that predominantly affects African-American and Hispanic populations. According to the CDC, sickle cell anemia impacts 1 out of 365 African-American people, and 1 out of 16,300 Hispanic people. As those populations are overrepresented in jails and prisons, it is essential that correctional health care professionals understand sickle cell anemia and the health needs of those who suffer from it.
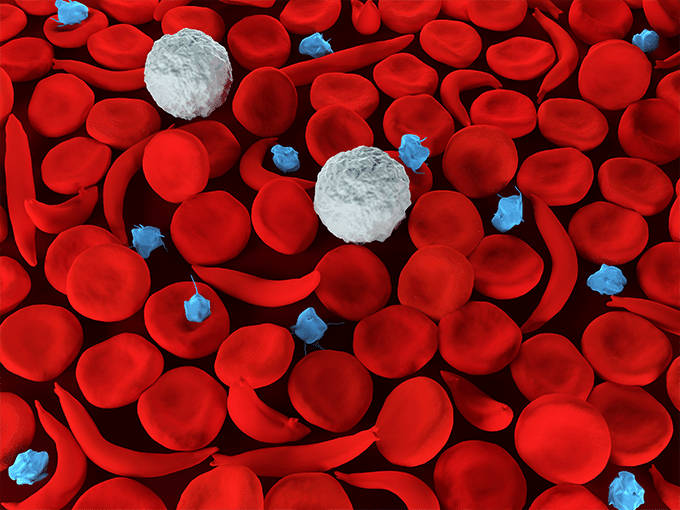
People with sickle cell anemia have a genetic mutation that causes some of the red blood cells to become misshapen, taking on a C or “sickle” shape, unlike healthy red blood cells that are round. The main manifestations of the disease are pain, infection, and fatigue.
Treat Pain to Prevent Complications
People with sickle cell anemia can experience extreme pain in a flare of illness called a “pain crisis.” The pain crisis is brought on by a blockage of blood vessels due to buildup of the sickled blood cells, which clump more easily than normally shaped round red blood cells. The intensity and duration of these pain crises can last anywhere from several hours to days. Patients can experience dozens of pain crises each year, often requiring hospitalization.
People with sickle cell anemia experience fatigue related to low red blood cell count, or anemia, as the sickled red blood cells die after 10-20 days in the circulation, compared to normal red blood cells that last 120 days. This shortage of red blood cells prevents organs from getting enough oxygen, causing fatigue.
Undertreatment of pain in people with sickle cell anemia has been documented in the literature. Several studies show that clinicians think people with sickle cell anemia over-report their pain, leading to less than adequate care.
But adequately treating pain is the standard of care. More than just symptom management, pain treatment is part of essential care to ensure positive patient outcomes and reduce the risk of more severe complications like heart attack and stroke.
There are other serious complications as well. Sickled red blood cells can damage the spleen, which puts patients at risk for recurring infections. Patients are also at an increased risk for stroke, due to the increased likelihood of clot formation, and for Acute Chest Syndrome, a period of pain and respiratory distress caused by the congregation of sickled cells in the small blood vessels of the lungs.
Care for Sickle Cell Anemia in Corrections
Given the chronic nature and preponderance of sickle cell anemia, correctional facilities are advised to develop protocols and guidelines for both acute and long-term treatment of patients with the disease.
- At intake, ask about a diagnosis of sickle cell anemia.
- For those with sickle cell anemia, find out what medications they are on. The main treatment is a medicine called hydroxyurea which, when taken daily, can reduce the occurrence of pain crises as well as the need for blood transfusions and hospitalizations. Opioid-based medications, including oxycodone, morphine, and hydromorphone, are currently the standard of care when treating acute sickle cell crises. Research is seeking to identify alternatives to opioid medications, particularly for patients with a history of opioid use disorder.
- Develop an individualized care plan that incorporates any previous plan and medications and details management of the individual’s pain crises. Ideally, the plan will take the patient’s preferences into account and ensure consistency of care if the patient is seen by different providers. If possible, refer to a hematologist.
- Intravenous fluids and oxygen therapy also should be provided to patients undergoing an acute crisis. Pharmaceutical-grade L-glutamine and crizanlizumab are recently approved drugs that reduce the frequency of pain crises. Voxelotor, another recently approved drug, can help reduce fatigue and anemia. Those medications should be continued for any patients who were prescribed them prior to incarceration.
- Ensure access to accommodations for adequate warmth (blankets and heating pads) and hydration during the length of the patient’s incarceration. Cold temperatures and dehydration both increase the severity of symptoms.
- Include continuity of care in discharge planning. Ensure that the incarcerated individual knows where to access care in the community and will have access to medications.
Currently, bone marrow transplant is the only cure for sickle cell anemia, though it is difficult for patients to find a matching donor. Genetic therapies are also being explored, although none have yet received FDA approval.
Nicole Cassarino is a student at Tufts University School of Medicine; Yoseph Boku is a student at Harvard University School of Medicine.