
Standards Q&A: 75% Custody Health Training Requirement
Does the 75% requirement refer to all custody staff or only those working during
Home Self-Injurious Behaviors in Correctional Facilities, Part 1
 May 11, 2022
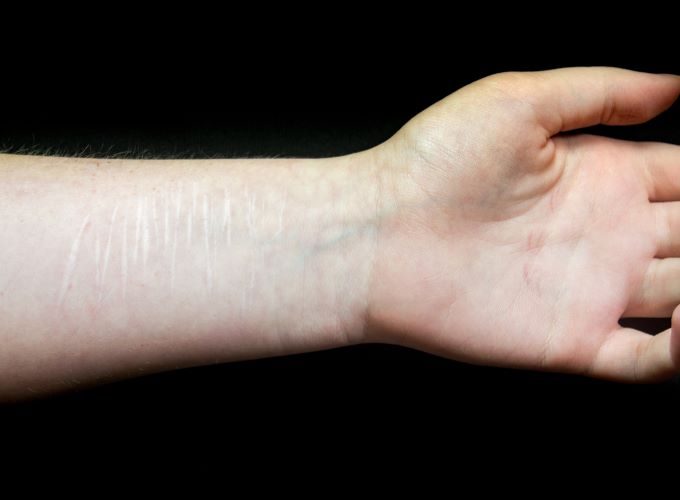
May 11, 2022“Inmate swallowed a piece of metal from her wristband” … “Patient used a metal piece to cut her arm” … “IM banged his head against the cell window, sustaining a 2 cm laceration” …
Those notes may sound familiar…and anxiety-inducing. Self-injurious behaviors – acts intended to cause bodily harm but not death – are all too common in correctional settings. Recent studies of 20 countries show that the annual prevalence of self-harm in prisons far exceeds that in the community, especially among women. Self-injurious behaviors are a significant challenge for correctional health professionals, and a leading cause of morbidity in the incarcerated population.
Other terms for self-harm include nonsuicidal self-injury, self-mutilation, self-directed violence, and parasuicide. Common examples include cutting, head banging, self-biting, burning, and ingesting or inserting foreign objects. Despite nonsuicidal intent, self-injurious behaviors don’t always have a distinct demarcation from suicidal behaviors, and a lack of suicidal intent doesn’t eliminate the potential for lethality. The ability to distinguish between the two can be difficult, as some self-injurious behaviors inadvertently cause death.
Self-Harm Risk Factors and Related Diagnoses
Three strong risk factors for self-harm among incarcerated populations include homelessness, unemployment prior to incarceration, and age younger than 30 years. Other leading risk factors include a lengthy sentence, a history of childhood sexual abuse, a family history of suicide and self-injury, and being young, single, and female.
The experience of early childhood trauma (including emotional, sexual, and physical abuse) and violence in adulthood are linked to self-injurious behaviors, particularly for women. Low levels of social support compound the risks.
Diagnoses commonly associated or co-existing with nonsuicidal self-injurious behaviors include cluster B and C personality disorders, major depression, and other mood, psychotic, cognitive, and developmental disorders, each with distinguishing characteristics.
The most common diagnosis is borderline personality disorder. For those with BPD, self-injury is considered to reduce painful emotions; relieve anger, distress, or dysphoria; or counteract dissociative states.
More extreme acts of self-injury tend to occur most commonly with psychotic conditions. The acts and damage can be severe and include significant tissue damage or loss of organ functioning, such as enucleation of an eye, amputation, or genital mutilation.
Head banging, scratching, hitting, and hand biting are also seen among those with intellectual disabilities. Hair pulling occurs with trichotillomania, skin picking with excoriation disorder, and other acts with a factitious disorder such as Munchausen syndrome (in which someone deceives others by appearing sick, by purposely getting sick, or by self-injury).
Links also exist between drug use and self-harm, given the less conscious control of actions while intoxicated or during withdrawal.
Why Do People Self-Harm?
Emotional dysregulation tends to be the most frequent reason for self-harm; self-injury is used as an attempt to release or cope with strong emotions. Incarcerated individuals can have other motives for self-harm that may have little to do with emotional or psychiatric disorders. The environment often plays a role, and interpersonal conflicts with staff or other incarcerated individuals sometimes precipitate self-injury. Self-injurious behaviors may establish a sense of autonomy and control or serve as a coping mechanism, a form of retaliation, a way to communicate anger, or a tool for secondary gain. Antecedent emotions often include anger, anxiety, or boredom, followed by relief or calm after the act, which can increase the likelihood of recurrence.
The highest rates of self-injurious behaviors have been found to occur in isolation, segregation, solitary confinement, and other lockdown units that impose deprivations, including disciplinary infractions. Given that extreme conditions of confinement can result in significant psychological distress, physical pain may provide a distraction from psychological pain. The staff response then provides human contact, paradoxically and inadvertently reinforcing those behaviors with attention, change in housing, diversion, or access to certain medications.
Kavita Khajuria, MD, is a forensic psychiatrist in clinical practice at Twin Towers Correctional Facility in Los Angeles, California.
Part 2, Management and Treatment Interventions.
Learn about NCCHC’s Correctional Mental Health Care Conference, coming up August1-2 in Denver.
For guidance about best mental health practices in corrections, refer to NCCHC’s Standards for Mental Health Services.
Go the extra mile and earn mental health accreditation from NCCHC.
If you’re a correctional mental health professional, advance your career with CCHP-MH certification.


